36: Pediatric Urogynecology
This chapter will take approximately 8 minutes to read.
Introduction
Urogynecologic complaints are commonly encountered in any pediatrician’s practice. Investigation of those complaints may uncover a variety of problems, ranging from benign to pathologic and from behavioral to congenital. Often, genital and urologic complaints in girls are inseparable, and some gynecologic concerns warrant evaluation of the urologic tract as well. In this chapter, we cover some of the more common urogynecologic problems that a clinician may encounter in his or her practice.
Skene’s Gland Cysts
Skene’s, or paraurethral glands are the female counterpart to the male prostate gland. Arising laterally in the distal urethra, they may become obstructed, resulting in a cyst. While more common in adults, they may occur in young girls as well.1 On physical exam, a thin-walled, tense cystic mass may be seen bulging from one side or the other of the urethral meatus. This may be differentiated from urethral prolapse, which results in circumferential bulge from the meatus, or prolapsed ureterocele, which is a cystic mass bulging from the lumen of the urethral meatus. Diagnosis may be made on physical exam alone, but in cases where urinary tract obstruction or ureterocele need to be ruled out, ultrasound may be obtained. Management is typically conservative, as most will spontaneously regress.2 Less commonly, surgical excision may be required.1,2
Bartholin Gland Cysts
Bartholin glands in females correspond to the bulbourethral glands in males and are found bilaterally in the labia minora at 4 and 8 o’clock.3 This is a mucus-secreting gland, aiding in vaginal lubrication. When obstructed, a cyst may form. Again, these are more common in adults, but they may be noted in children. Incidence increases with age until menopause.4 Exam will reveal a bulge or cystic structure on the lateral wall of the vulva, deep to the bulbospongiosus muscle. Again, the preferred management is conservative.2
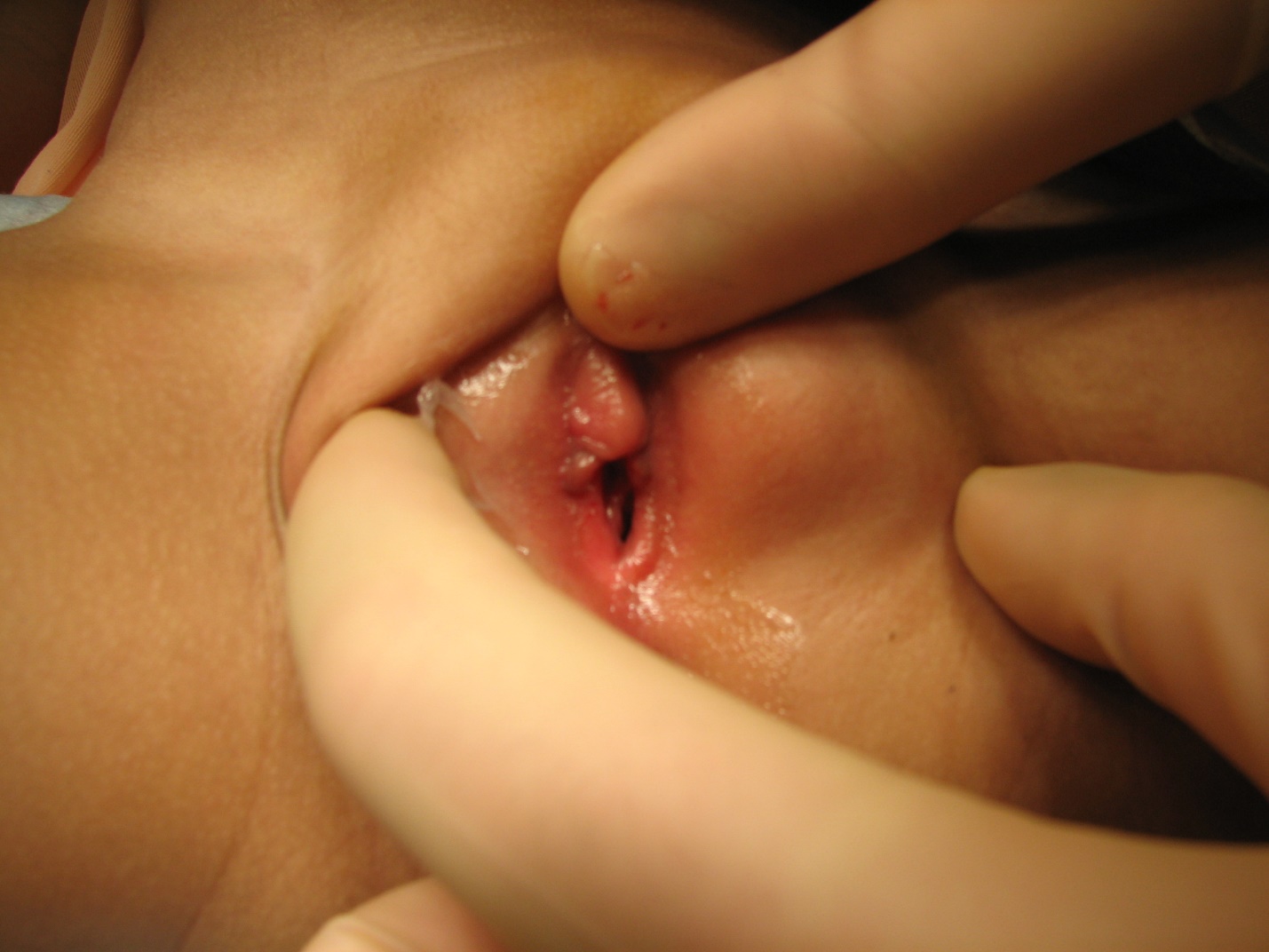
Figure 1 Bartholin gland cyst in young girl with cystic mass arising from left labial wall
Prolapsed Ureterocele
A ureterocele is a saccular outpouching of the distal ureter through the muscular wall of the bladder. Many ureteroceles are found in the setting of duplicated renal collecting system. Hydronephrosis may result due to obstruction or vesicoureteral reflux. Indeed, about 50% of ureteroceles will have ipsilateral reflux and about 25% will be associated with reflux on the contralateral side. For that reason, voiding cystourethrogram is a crucial step in the workup of a ureterocele.2 With the advent of prenatal ultrasound screening, many ureteroceles are discovered in the workup for perinatal hydronephrosis. Depending on the size of the outpouching, the ureterocele may prolapse through the urethra, particularly in females, which will appear as a smooth, mucosal-covered mass bulging from the lumen of the urethra.5 Discovery should result in prompt referral for treatment, of which the mainstay is surgical incision and/or excision.6,7,8 In some more severe cases, bladder neck reconstruction and/or ureteral reimplantation may be required.2
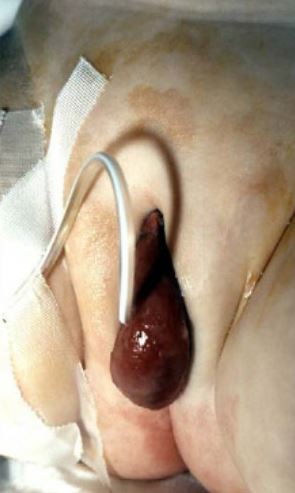
Figure 2 Prolapsed ureterocele with catheter in place
Imperforate Hymen
In normal neonatal development, the hymen, thin epithelial membrane, should spontaneously rupture. If it fails to do so, the result is an imperforate hymen, which commonly presents as a pubertal girl with amenorrhea and cyclic abdominal pain.9 Patients may also present as neonates due to ongoing circulation of maternal estrogen. This causes production of cervical mucus, whose buildup in the vagina and uterus results in hydrocolpos or hydrometrocolpos.2 Presentation can vary, including complaints of perineal mass, urinary retention,10 acute abdominal pain mimicking appendicitis,11 or chronic abdominal pain.12 Hydronephrosis has also been observed.13,14 On physical exam, the classic finding is a perineal bulge. Incision of the hymen is the definitive treatment, but clinicians should also be alert to the possibility of urinary retention, caused by mass effect on the bladder outlet with resulting obstruction, and place urethral catheter in that scenario.2,9 Clinicians should also avoid the temptation to simply aspirate or make a small incision for symptomatic relief, as pelvic inflammatory disease has been documented and recurrence is likely.5,9
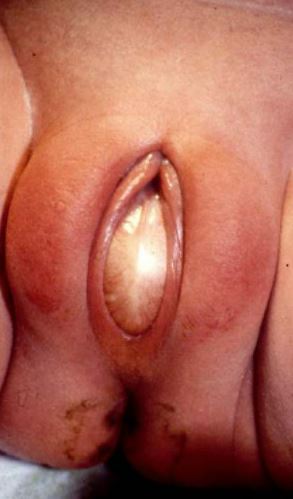
Figure 3 Imperforate hymen with bulging membrane
Labial Adhesions
Labial adhesions refer to the fusion of the labia minora. It typically starts at the posterior fourchette and progresses anteriorly to varying degrees. These are thought to occur due to low circulating estrogen levels in prepubertal girls.5 In many girls, the adhesions are asymptomatic, but they may also present with vulvovaginal discomfort and irritation, pain with wiping, or post-void dribbling, which occurs due to pooling of urine behind the adhesions. Asymptomatic adhesions can be managed conservatively, as 80% will resolve spontaneously within a year. Parents should be counseled on good perineal hygiene.2,5,15 The mainstay of medical treatment remains topical estrogen cream, which has been proven to be superior to topical emollients.5,16 Less commonly, mechanical separation under local or general anesthesia may be required. Parents should be informed that recurrence is common, up to 15%, and should be educated on the importance of regular separation of labia after successful treatment to prevent that recurrence..2,5,15 Of note, parents should avoid aggressive separation of the labia as gentle application of pressure when applying topical emollients is enough to prevent recurrence and not traumatic.
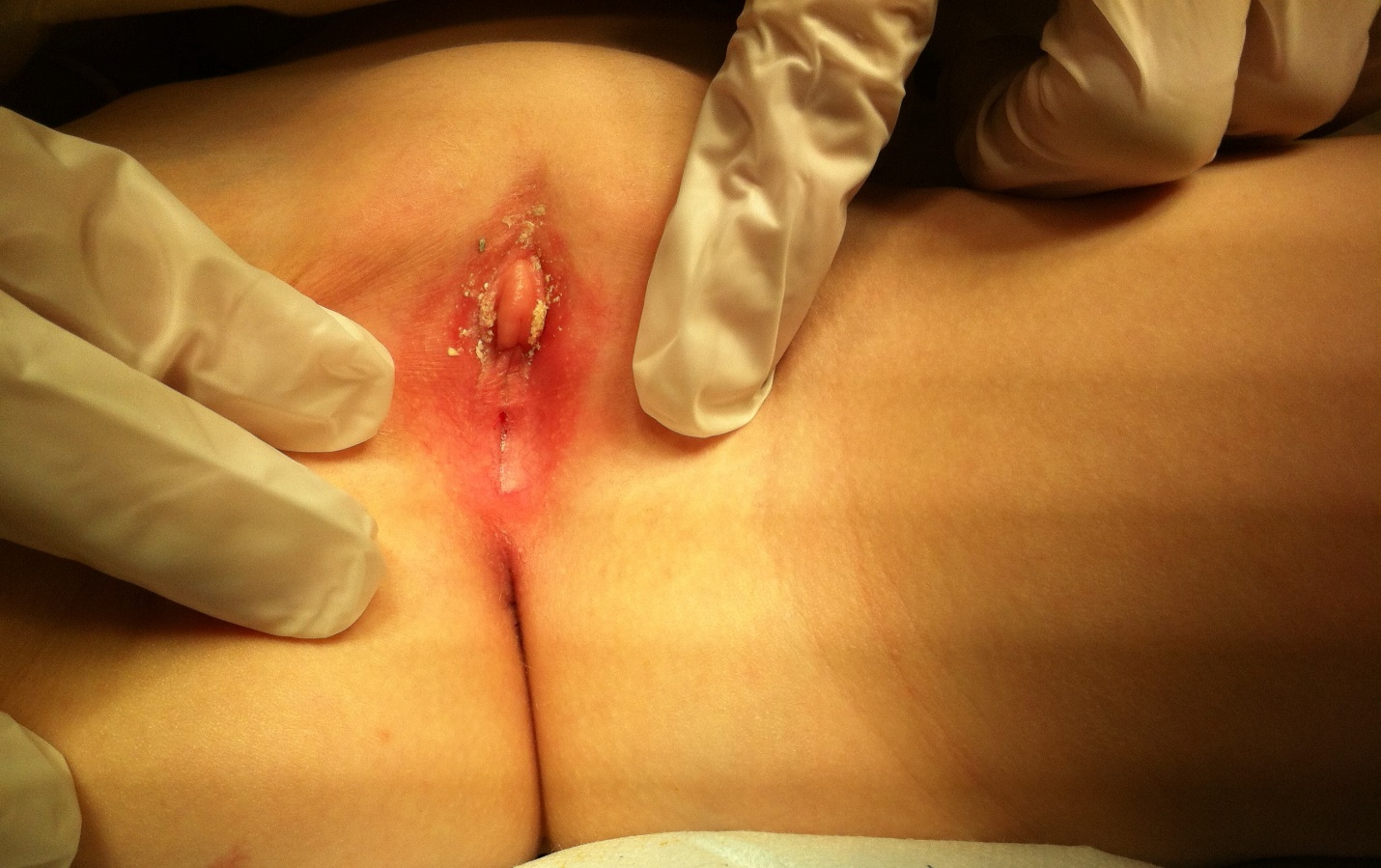
Figure 4 Examples of labial adhesions
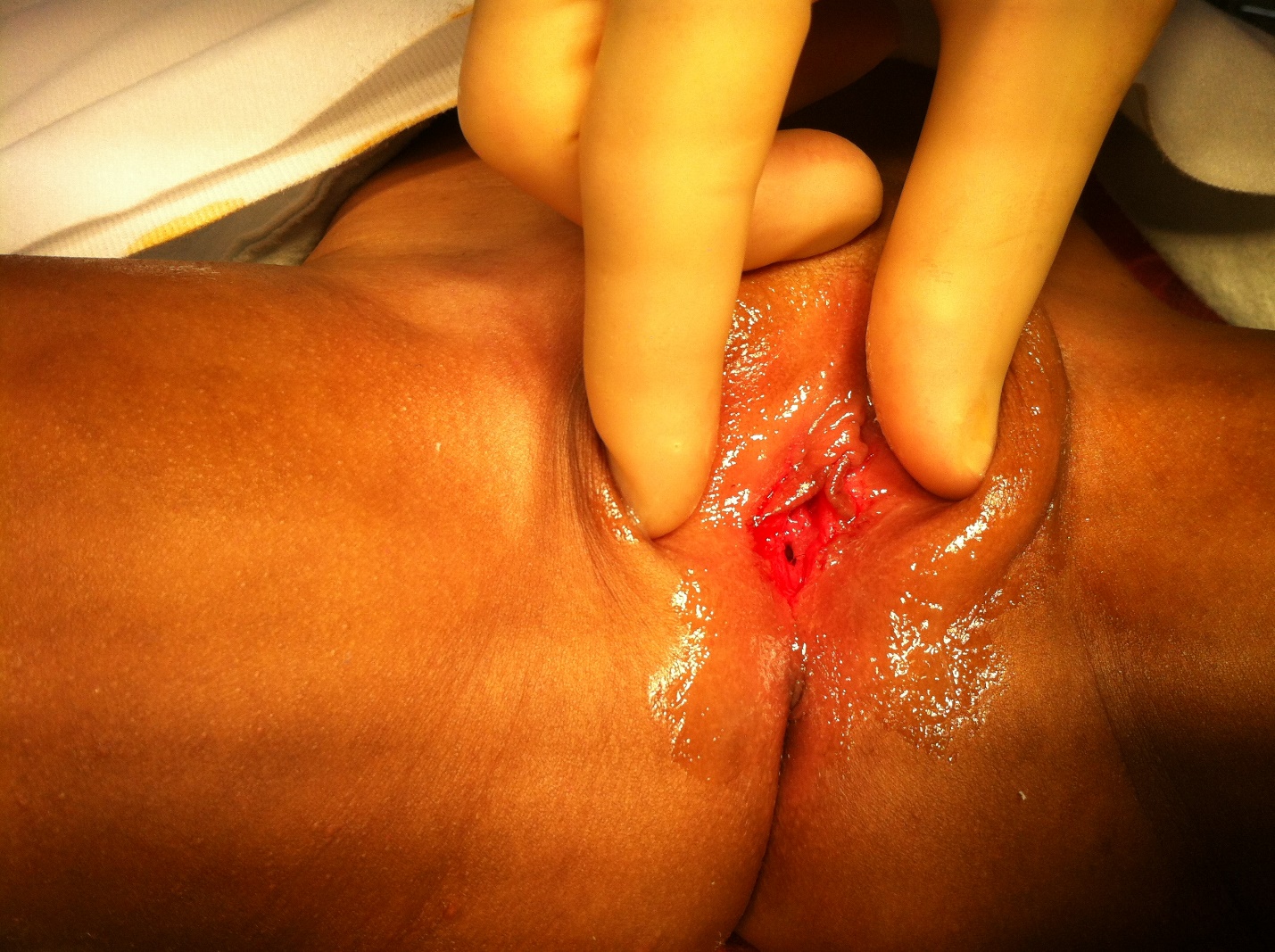
Figure 5. Examples of labial adhesions
Urethral Prolapse
Urethral prolapse presents as a circumferential bulge from the urethral meatus. It is a rare condition that is seen more frequently in black girls, for unknown reasons, and post-menopausal women. The exact incidence is not well known, as many patients likely have little-to-no symptoms and never seek care. Estrogen deficiency has been proposed as a possible etiology. This can lead to atrophy of the distal urethra, and, with increased intra-abdominal pressure, the distal urethra may prolapse. It can also be seen after peri-urethral injections. The exposed urethral mucosa may become inflamed and friable, resulting in symptoms such as pain, dysuria, discharge, and bleeding or hematuria. Medical management with topical estrogen cream and sitz baths is preferred. Topical steroids have also been used. Excision of the prolapsed portion of the urethra is reserved for more extreme cases..2,5,17 In majority of the cases, ensuring good bowel habits to minimize severe straining is key to a more long-term success without any further recurrences.
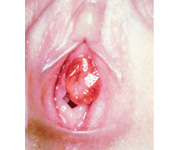
Figure 6 Circumferential prolapse of the urethra in a young girl
Lichen Sclerosus
While lichen sclerosus stereotypically affects adults, particularly middle-aged women, it can also affect young girls, with a peak incidence noted at ages 4-6 that accounts for 7-15% of all cases.18 Presenting symptoms include pruritus, vulvar discomfort or discharge, bleeding, dysuria, and bowel and bladder dysfunction. Physical exam reveals white, shiny skin plaques. The stereotypical configuration is “figure-of-8”, involving the vulva and perianal region. Treatment involves strong topical steroids, with the goal of preventing atrophy and introital narrowing in addition to symptomatic relief. While there is some association with malignancy in adults, this has not been observed in children. There is thus little role for biopsy in children. However, long-term, regular follow-up is important.2,18
Müllerian Agenesis
Müllerian agenesis is the failure of the Müllerian duct to develop into the fallopian tube, uterus, cervix and upper 1/3 of the vagina, resulting in varying absence of those structures. The most common presentation is amenorrhea. On physical exam, varying amounts of vaginal atresia may be observed. Differential diagnosis should include disorders of sexual development with 46,XY karyotype, such as complete androgen insensitivity or 5-alpha reductase deficiency. Therefore, workup should involve karyotype and pelvic ultrasound to evaluate for uterus, ovaries, and cervix.5 It may be associated with renal abnormalities, such as renal agenesis, so renal ultrasound should also be obtained. Once diagnosis is confirmed, surgical reconstruction can involve vaginal dilation, vaginoplasty, or even creation of a neovagina with bowel.2
Vulvovaginitis
Vulvovaginitis is a term used to cover a wide variety of presentations of inflammation of the vulva and vagina. Vulvovaginitis is one of the most common gynecological complaints in our pediatric female population.19 There is a wide range of etiologies for vulvovaginitis, and management depends on the underlying cause. Furthermore, as girls age and their physiologies change, the prevalence of certain etiologies changes. In young girls, a hypoestrogenic environment results in thin vaginal and vulvar epithelium with few lactobacillus species, resulting in a more neutral pH. With puberty, increasing estrogen stimulates a more protective environment, with more mature epithelium and a more acidic pH. Female anatomy is also important. The proximity of the vagina to anus can lead to fecal flora into the vagina, especially in young children and children with bowel and bladder dysfunction. As such, the clinician should pay attention to bowel and bladder habits, paying particular attention to signs of constipation. The clinician should remember that diarrhea may be evidence of encopresis and consider KUB to evaluate for constipation if any evidence of bowel or bladder dysfunction is present. Other contributing anatomic and behavioral features in the female child include lack of labial fat pad or pubic hair, small labia minora, and tendency to explore their bodies with transfer of respiratory bacteria to the perineum.20 Foreign bodies, local irritants such as tight underwear, bath soaps, laundry detergents, and atopic skin conditions, such as other allergies or eczema, should be considered in all age ranges. Sexual abuse and sexually transmitted diseases are more common etiologies in older, adolescent girls but should also be considered in all age ranges. Evaluation starts with a thorough history, but the mainstay of diagnosis is a good physical exam. Normally, pulling the labia majora forward and out, rather than simply spread apart, gives great visualization for the external genitalia, including the labia minora, urethra, and vaginal introitus. Management strategy is dependent on the potential causes. If yeast or bacterial infections or sexually transmitted infections are suspected, those should be treated appropriately with antimicrobials. However, majority of the cases are due to nonspecific etiology and good hygiene methods are recommended.19 Possible offending agents, such as tight underwear or irritating soap should be discontinued. Bowel and bladder dysfunction should be addressed, typically with relief of constipation by oral bowel regimen or bowel cleanout, as necessary.
References
- Foster J, Lemack G, Zimmern P. V2-06 Skene’s Gland Cyst Excision. J Urol 2016; 193 (4s): 817–820. DOI: 10.1016/j.juro.2015.02.331.
- Jeremy West AA, Cooper. Urogynecology". In: Greenfield SP, C.S., editors. Pediatric Urology for Primary Care. 2019. DOI: 10.1097/01.aog.0000231943.71829.0d.
- Omole F, K.R. P, K C, K.. Incision and Drainage of Bartholin Gland Duct Cyst or Abscess with Word Catheter Placement; Marsupialization of Bartholin Gland Duct Cyst or Abscess. Operative Dictations in Pediatric Surgery 2019; 99 (12): 217–218. DOI: 10.1007/978-3-030-24212-1_53.
- Lee WA, Wittler M. Bartholin Gland Cyst. Treasure Island, FL, USA: StatPearls Publishing; 2022, DOI: 10.53347/rid-26348.
- Wein AJ. Campbell-Walsh-Wein urology. Twelfth edition review., Philadelphia: Elsevier, Inc; 2020, DOI: 10.1055/a-1307-2419.
- Pogorelić Z, Todorić J, Budimir D, Saraga M. Laser-puncture of the ureterocele in neonatal patients significantly decreases an incidence of de novo vesico-ureteral reflux than electrosurgical incision. J Pediatr Urol 2021; 17 (4): 492.e1–492.e6. DOI: 10.1016/j.jpurol.2021.02.028.
- Nguyen DH, Brown CT. Puncture of prolapsed ureterocele at bedside without anesthesia or sedation. J Pediatr Urol 2020; 16 (3): 390–391. DOI: 10.1016/j.jpurol.2020.03.011.
- Tanneru K, Pichandi RE. A Rare Case of Prolapsed Ureterocele With Large Redundant Flap After Unroofing in Adult Female. Urology 2021; 147: 35–36. DOI: 10.1016/j.urology.2020.07.031.
- Abdelrahman HM, Feloney MP. Imperforate Hymen. Treasure Island, FL, USA: StatPearls Publishing; 2022, DOI: 10.1056/nejm191005051621806.
- Goto K. Acute urinary retention in two adolescent girls with imperforate hymen. J Obstet Gynaecol Res 2019; 45 (3): 739–742. DOI: 10.1111/jog.13875.
- Amponsah-Manu F, Ssentongo P, Arkorful T, Ofosu-Akromah R, Ssentongo AE, Hansen-Garshong S, et al.. Imperforate hymen and leaking hematosalpinx mimicking acute appendicitis: A report of a rare case and a review of literature. Int J Surg Case Rep 2019; 63: 69–74. DOI: 10.1016/j.ijscr.2019.09.003.
- Chia M, Ho C. Missed diagnosis of imperforate hymen later presenting with hypertension. BMJ Case Rep 2020; 13 (9): e237416. DOI: 10.1136/bcr-2020-237416.
- Peleg D, Shinwell ES. Newborn Imperforate Hymen Resulting in Hydronephrosis. J Pediatr 2019; 207: 258. DOI: 10.1016/j.jpeds.2018.12.051.
- Zhang M, Luo Y, Wang S, Wang S, Kuang H. A case report of hydronephrosis caused by imperforate hymen in an infant. Medicine (Baltimore) 2020; 99 (45): e23072. DOI: 10.1097/md.0000000000023072.
- Gonzalez D, Anand S, Mendez MD. Labial Adhesions. 2022. DOI: 10.1542/9781610020473-part07-ch282.
- Dowlut-McElroy T, Higgins J, Williams KB, Strickland JL. Treatment of Prepubertal Labial Adhesions: A Randomized Controlled Trial. J Pediatr Adolesc Gynecol 2019; 32 (3): 259–263. DOI: 10.1016/j.jpag.2018.10.006.
- Afolayan P, Abdel Goad EH, Pepu B. Traumatic catheterization as a precipitating factor for urethral prolapse in 4 years old child. Urol Case Rep 2020; 32: 101159. DOI: 10.1016/j.eucr.2020.101159.
- Orszulak D, Dulska A, Niziński K, Skowronek K, Bodziony J, Stojko R, et al.. Pediatric Vulvar Lichen Sclerosus–A Review of the Literature. Int J Environ Res Public Health 2021; 18 (13): 7153. DOI: 10.3390/ijerph18137153.
- Loveless M, Myint O. Vulvovaginitis- presentation of more common problems in pediatric and adolescent gynecology. Best Pract Res Clin Obstet Gynaecol 2018; 48: 14–27. DOI: 10.1016/j.bpobgyn.2017.08.014.
- Joishy M, Ashtekar CS, Jain A, Gonsalves R. Do we need to treat vulvovaginitis in prepubertal girls? Bmj 2005; 330 (7484): 186–188. DOI: 10.1136/bmj.330.7484.186.
Last updated: 2025-09-25 12:10